This information is for you if you have been offered or have had LLETZ.
It may also be helpful if you are a partner, family member or friend of someone in this situation.
Please note: This information was developed in collaboration with Jo’s Cervical cancer trust, which closed on 23rd May 2024. All links to the Jo’s cervical cancer trust website have been removed.
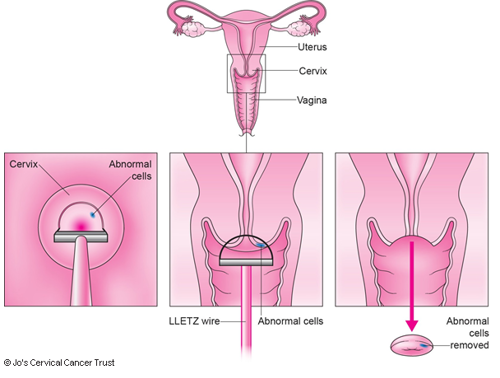
LLETZ stands for large loop excision of the transformation zone. It is a treatment to remove cell changes (abnormal cells) in the cervix.
This guide is for you if you have been offered or have had LLETZ. It may also be helpful if you are a partner, family member or friend of someone in this situation.
Within this information and accompanying leaflet we may use the terms ‘woman’ and ‘women’. However, it is not only people who identify as women who may want to access this leaflet. Your care should be personalised, inclusive and sensitive to your needs whatever your gender identity.
Key points
- LLETZ is a common treatment to remove cervical cell changes. It is usually done in an outpatient clinic in a hospital, using a local anaesthetic.
- After the anaesthetic has worn off, you may experience pain, vaginal bleeding and changes to vaginal discharge. This usually lasts between a few days and 4 weeks
- The benefit of LLETZ is that it can stop cell changes potentially developing into cervical cancer. It is successful in over 9 in 10 (over 90%) cases, meaning no further treatment is needed.
- Possible risks of LLETZ include an increased risk of late miscarriage or premature birth and cervical stenosis (narrowing of the cervix).
- If you have any physical or emotional effects after LLETZ, it is important to speak with your doctor or nurse so they can give you support.
About intimate examinations
The nature of gynaecological and obstetric care means that physical examinations are often necessary. This may involve an examination of your abdomen or an internal examination of your vagina.
We understand that for some women, including those who have experienced trauma, physical or sexual abuse, such examinations can be very difficult. Your healthcare professionals are there to provide kind and personalised care to you. If you choose not to be examined, they can discuss alternative options with you.
After explaining to you about the physical examination you are being offered, your healthcare professional will seek your consent. You should always be offered a chaperone. This could be a partner, family member, friend, support person or another healthcare professional.
If you feel uncomfortable, anxious, distressed or in pain at any time before, during, or after an examination, please let your healthcare professionals know, as they are there to support you.
If you find this difficult to talk about, you may communicate your feelings in writing or with the support of someone you wish to accompany you.
You can ask your healthcare professional to stop at any time during your physical examination.
Colposcopy
After cervical screening (a smear test), you may be invited to a colposcopy appointment. You are usually invited if your result shows human papillomavirus (HPV) and cervical cell changes.
Colposcopy is where:
- the grade of the cell changes are diagnosed – for example, low-grade or high-grade
- cell changes may be monitored or treated.
This is important because there is a chance of these cell changes developing into cervical cancer without monitoring or treatment.
You will meet a doctor or nurse called a colposcopist. They will use a type of microscope with a light at the end, called a colposcope, to take a closer look at your cervix. They may offer you tests to help diagnose cell changes and decide whether you need treatment, including:
- using different liquids to stain your cervix and show up any cell changes
- a biopsy, where a small piece of cervical tissue is removed – it is then sent to the lab for testing
If you need treatment, it may be offered during your first colposcopy appointment or you may be invited back to have treatment at another appointment. The option you are offered may be due to what the colposcopy tests show and your colposcopist. Both options are as good as each other.
If you are offered treatment during your first appointment, it is okay to ask for time to think about it either at the appointment or at home. Your colposcopist should invite you to have a seat away from the examination bed to talk you through the treatment and any questions. This is sometimes called see and treat.
Making a decision about treatment
Before you make a decision about treatment, it is important to understand the procedure, including benefits, risks and possible effects. Your colposcopist should explain these to you and give you the chance to ask any questions. You may also want to talk over your options with your family or friends.
It can help to write a list of questions and take it to your appointment.
You might like to ask some of the following questions:
- What types of treatment can I have?
- What does the treatment do?
- What could happen if I choose not have treatment?
- How long will the treatment take?
- Do I need to bring anything to the appointment?
- Will I be able to get home by myself after treatment?
- What physical effects might I experience after treatment?
- What emotional effects might I experience after treatment?
LLETZ is the most common treatment for cervical cell changes. It uses a thin wire loop with an electrical current to remove the affected area of the cervix.
Your appointment
Your appointment will happen in a colposcopy clinic at a hospital. You usually have LLETZ as an outpatient. This means you have it in a hospital examination room, but can go home afterwards.
You usually have a local anaesthetic for LLETZ. But you can choose to have it done under general anaesthetic, where you are asleep. If you would prefer this, talk to your colposcopist about the risks and benefits before your appointment.
If you take blood thinning medication or have a condition that affects your blood, it is important to tell your colposcopist before your appointment. You may have a higher risk of bleeding after the treatment (see below for further information on bleeding).
LLETZ treatment
You will have LLETZ lying on your back on an examination couch. The examination couch is adjustable and hoists are usually available if you need assistance.
Preparing for treatment
Like during cervical screening, your colposcopist will gently put a clean speculum into your vagina. Speculums come in different sizes so, if you find the standard size uncomfortable or painful, you can ask for a smaller one.
Your colposcopist will inject a local anaesthetic into your cervix. This means you are awake, but the area that needs treating is numb (you can’t feel it). The injection might sting for a short time and you may be aware of your heart beating faster. This feeling should pass within a couple of minutes.
You may also have a sticky pad put onto on your leg. This makes sure the electric current in the wire loop doesn’t burn you.
Before starting the treatment, your colposcopist will touch your cervix to check it is numb.
Having the treatment
Once your cervix is numb, your colposcopist uses the loop to remove the area of your cervix that has cell changes. It is normal to notice a slight burning smell and hear a noise like a soft vacuum cleaner.
The loop cuts the tissue and then another small instrument is used to seal the cut. This should not be painful, but you may feel some pressure. The treatment usually takes less than 2 minutes.
The cells and tissue that has been removed is sent to a laboratory:
- The test will check what kind of cell changes you had.
- The test will check whether cell changes have been completely removed. This is done by testing for an ‘edge’ of healthy cells around the area that was removed. This is sometimes called having clear margins.
After the treatment
Once the anaesthetic has worn off, you may have some bleeding. Your colposcopist should offer you a period pad to use, but you might like to bring your own. Do not use tampons or menstrual cups that you put into your vagina.
“Whilst the day of the treatment was frightening, the wonderful nurses and incredible women I met who were having similar experiences to me made things much more bearable. We spoke about our cervixes as comfortably and as naturally as if we were discussing TV. I will forever be grateful to the inspiring ladies I met that day.”
Nina, who had LLETZ for CIN3 and CGIN
You may have some physical effects after LLETZ (see below for further information). These usually last up to 4 weeks. Until these have stopped, it is best to avoid:
- tampons or menstrual cups – you can use a period pad instead
- penetrative vaginal sex – including fingers, tongues and other objects
- heavy exercise that causes you to sweat, such as running or a gym workout
- swimming
- long baths – you can continue to shower as normal.
Some travel insurance companies will not provide health insurance straight after treatment, so try to wait for about 4 weeks after treatment before going on holiday or flying. Any effects will usually have stopped by then. If you have a holiday planned, you can discuss dates for treatment with your colposcopist.
If you have any questions about what you can and can’t do after LLETZ, speak with your colposcopist.
After LLETZ, you will be invited for a follow-up appointment at your GP surgery or the colposcopy clinic. This should happen 6 months after the treatment.
At this follow-up appointment, you will have a test of cure. This is like cervical screening, where a sample of cervical cells is tested for high-risk HPV.
“The wait for the LLETZ result was mentally tough, especially in the 4 days after treatment when I fell ill with an infection. I'm so very lucky to have an incredible network of family and friends to rely on. The Jo's forum was full of women sharing similar experiences and this was immensely helpful to read.”
– Lisa, who had LLETZ for CIN3
LLETZ is usually successful and over 90 in 100 (90%) people do not have cell changes again. Fewer than 10 in 100 (10%) people will have cell changes again.
The benefit of LLETZ is that it prevents potential cervical cancer from developing which, in many cases, will outweigh the risks. However, like all treatments, LLETZ has risks and you may have some physical or emotional effects because of the treatment.
Talk to your colposcopist before treatment if you are worried about any risks. They can answer your questions and give you support. After treatment, your GP or a specialist doctor will be able to offer support.
Bleeding
About 85 in 100 (85%) people experience bleeding after LLETZ. About 15 in 100 (15%) people do not experience bleeding. This is expected after LLETZ and can last between 2 days to up to 4 weeks.
You may have bleeding because of the soft scab that forms on the cervix where the cells were removed. This may bleed while it heals.
The bleeding is usually like a period, but may be slightly heavier than your normal period. About 10 days after treatment, the bleeding may get heavier. This is common and a sign that the scab is healing. Your first period after treatment may be slightly heavier or out-of-sync with your regular cycle.
Important! If you are on blood thinning medication or you have a haematological condition, you must tell your colposcopist because you may have a higher risk of bleeding after LLETZ. If the bleeding is soaking through a period pad every hour, call the contact number given by your colposcopy team or call 111 out of hours. This is sometimes called delayed haemorrhaging. The hospital team or 111 will be able to advise you and make sure you get the right care.
Pain
About 67 in 100 (67%) people experience pain after LLETZ. About 33 in 100 (33%) people do not experience pain.
Some pain is expected for between 2 days to up to 4 weeks after treatment. The pain varies from person to person, but should not be too severe. It is often described as a cramping pain, like a period. You can talk to your doctor about over-the-counter medication that should help.
Important! Some people may experience pain for longer, but it usually goes away within 3 months. If you are in a lot of pain or find it is affecting your day-to-day life, talk to your GP. They can advise on pain medication, offer reassurance based on your medical history and, if needed, will be able to check you are healing properly.
Changes to vaginal discharge
About 65 in 100 (65%) people have changes to their vaginal discharge. About 35 in 100 (35%) people don’t have any changes to their vaginal discharge.
Changes to vaginal discharge can last for about 4 weeks. Straight after treatment, you may have a watery, brown vaginal discharge.
About 10 days after treatment, you may notice a coffee granule-like vaginal discharge. This is normal and a sign that the soft scab on your cervix is healing.
Important! Between about 1 and 14 in 100 (0.8% to 14%) people get an infection after LLETZ. Talk to your GP if your vaginal discharge smells bad, or is a yellow or green colour. If there is a chance you have an infection, you will be offered antibiotics.
Premature birth or late miscarriage
About 2 in 100 (2%) people who become pregnant at any time after LLETZ will give birth before 37 weeks (prematurely) because of the treatment. About 98 in 100 (98%) people will not give birth prematurely because of the treatment.
Giving birth prematurely is more likely if you have had LLETZ more than once or had more than 10mm of your cervix removed. Most LLETZ treatments remove less than 10mm of your cervix.
If you become pregnant after LLETZ, tell your doctor or midwife that you have had the treatment. They may refer you to a specialist in preventing preterm birth.
Cervical stenosis
The opening of the cervix (the os) can narrow or close and become scarred after LLETZ. This is called cervical stenosis. If this happens, the passage between the womb and vagina may become partly or fully blocked. Research suggests there is between a 2 to 14 in 100 (2% to 14%) risk of this happening.
You are more likely to develop cervical stenosis if you:
- have been through menopause
- have had more than one treatment
- have had treatment that removes a large area of your cervix.
You may not have any symptoms of cervical stenosis. If you have periods, they might become irregular or painful. If you are trying to become pregnant, the sperm may not be able to get to the womb. It may also be harder for your doctor or nurse to do cervical screening in the future, but you can be referred to colposcopy if this happens.
Cervical stenosis can sometimes be treated with cervical dilators to help widen the cervix.
Jo’s Cervical Cancer Trust has spoken with women and people with a cervix who have had treatment for cervical cell changes to understand their experiences. In most cases, they had LLETZ for high-grade cell changes – CIN2 or CIN3. The figures in this section are taken from that research to help you feel as prepared as possible. It is important to remember that everyone heals at a different pace and will have a different experience after LLETZ.
Impact on your feelings
You may have strong feelings about what LLETZ means for your physical wellbeing and future. These feelings could be positive, such as relief that you have had treatment, but you may also feel worried about how your body will recover.
For the women and other people with a cervix that Jo's Trust spoke with:
- 86 in 100 (86%) had fears about cancer, while 14 in 100 (14%) did not
- 71 in 100 (71%) had anxiety after treatment, while 29 in 100 (29%) did not
- 45 in 100 (45%) had fears about their fertility, while 55 in 100 (55%) did not
- 24 in 100 (24%) experienced depression after treatment, while 76 in 100 (76%) did not.
All of your feelings and concerns, including any we don’t mention in this guide, are valid and it is important you get the right support to deal with them. Here are some of the ways you could get support.
Get support from loved ones
Some people find that a support network of friends and family helps their emotional recovery after LLETZ. There are lots of ways they can help, from talking your feelings through, to offering a distraction and positive presence.
Talk to your GP or another trusted doctor
Before, during and after LLETZ, you will be in the care of professionals who want to make the experience as good as possible for you. If you are worried about anything, talk to them so they can give you the right support and ease any concerns. Or, if you have another doctor you know and trust, ask to talk with them about any worries.
Get support from charities
There are many charities and organisations who offer support services so you can feel listened to and work through your feelings (see Other useful organisations at the end of this information). These services can also signpost to other places that may be able to help.
Ask for a referral to counselling
If you feel that expert support would help, you can self-refer or ask your GP to make a referral for NHS counselling. You can also make an appointment privately, for a cost. You can search for a private counsellor at bacp.co.uk/therapists.
Sex and relationships
You may experience sex and intimacy differently after LLETZ. This may also have an impact on your relationships. These differences may be because of physical changes, emotional changes, or both.
In the women and other people with a cervix that Jo's Trust spoke with, about 46 in 100 (46%) had changes to how they feel, while 54 in 100 (56%) did not. These changes included feeling less attractive or confident, as well as worries about passing on HPV.
Pain during or after sex
About 33 in 100 (33%) people had pain during or after sex, while 67 in 100 (67%) did not. In most cases, this pain lasted for less than 3 months. In some cases, pain during or after sex lasted for:
- between 3 and 12 months in 5 in 100 (5%)
- between 1 and 3 years in 6 in 100 (6%)
- between 3 and 5 years in 3 in 100 (3%)
- more than 5 years in 5 in 100 (5%).
Bleeding during or after sex
About 22 in 100 (22%) people had bleeding during or after sex, while 78 in 100 (78%) did not. In most cases, the bleeding lasted for less than 3 months. In some cases, the bleeding lasted for:
- between 3 and 12 months in 3 in 100 (3%)
- between 1 and 3 years in 3 in 100 (3%)
- between 3 and 5 years in 1 in 100 (1%)
- more than 5 years in 2 in 100 (2%).
Getting support
It is important to see your GP if you have any symptoms such as pain or bleeding. They can examine you and talk through ways to make it better, such as using more lubricant during sex to lessen any pain.
It may help to speak to a trusted person about any loss of confidence – whether that is a partner, family, friends, your GP, or other people who have had LLETZ. Talking through your worries might ease them or give you new ideas about how to handle them.
If you and a partner are struggling to reconnect after LLETZ, you may want to consider couples counselling. An unbiased expert can help you start and explore conversations around sex and intimacy, so you can find solutions together. You can self-refer through local NHS services, speak with your GP, or search for a local counsellor at bacp.co.uk/therapists.
Lasting pelvic pain
Some pelvic pain is expected for a couple of days after LLETZ, but you may have pain for longer. We don’t know if this is directly because of the treatment or because of other conditions or life events that have happened since treatment.
In the women and people with a cervix that Jo's Trust spoke with, pelvic pain lasted for:
- between 3 and 12 months in 5 in 100 (5%)
- between 1 and 3 years in 6 in 100 (6%)
- between 3 and 5 years in 3 in 100 (3%)
- more than 5 years in 5 in 100 (5%).
If you experience lasting pelvic pain, it is important to speak with a doctor. They can investigate the cause of the pain and offer the right support.
Rare effects
There is a small chance you may experience other effects after LLETZ. Jo's Trust spoke with a few women and people that had LLETZ who said their periods have permanently changed, cervical screening is more uncomfortable or they no longer feel the same sensations during sex. We don’t know if this is directly because of the treatment or other conditions or life events that have happened since treatment.
If you experience these effects, or anything we don’t mention in this guide, speak with your doctor or nurse. They will be able to offer you further support based on your individual circumstance.
Other useful organisations
The British Society for Colposcopy and Cervical Pathology (BSCCP)
The BSCCP has FAQs for women and people with a cervix about cervical cell changes, treatment and follow-up. www.bsccp.org.uk/women
British Association for Counselling and Psychotherapy (BACP)
The BACP has a list of registered counsellors, as well as a directory to help you find a counsellor in your area. www.bacp.co.uk/about-therapy/how-to-find-a-therapist
If you have experienced sexual violence, we understand that colposcopy may be very difficult. It may help to get support from an expert organisation, such as the ones we list below:
Rape Crisis England & Wales
Provides information and support to survivors of sexual violence, sexual assault and sexual abuse across England and Wales. www.rapecrisis.org.uk
Rape Crisis Scotland
Provides information and support to survivors of sexual violence, sexual assault and sexual abuse across Scotland. www.rapecrisisscotland.org.uk
Nexus NI
Offers free counselling for people who have experienced sexual violence, sexual assault and sexual abuse across Northern Ireland. http://nexusni.org
Thanks
Thank you to Jo's Trust for partnering with us to develop this information. Thank you also to all the experts who checked the accuracy of this information and the volunteers who shared their personal experience to help us develop it.
References
This information is based on literature searches and expert review. Here is a sample of the references used for this resource:
- Jo’s Cervical Cancer Trust (2019). Not So Simple: The impact of cervical cell changes and treatment. Available from www.jostrust.org.uk
- Public Health England (2020). Cervical screening: programme and colposcopy management. Available from www.gov.uk
- The TOMBOLA Group (2009). After-effects reported by women following colposcopy, cervical biopsies and LLETZ: results from the TOMBOLA trial. BJOG.
For more information about the references used, please contact info@jostrust.org.uk.
If you are asked to make a choice, you may have lots of questions that you want to ask. You may also want to talk over your options with your family or friends. It can help to write a list of the questions you want answered and take it to your appointment.
Ask 3 Questions
To begin with, try to make sure you get the answers to 3 key questions, if you are asked to make a choice about your healthcare:
- What are my options?
- What are the pros and cons of each option for me?
- How do I get support to help me make a decision that is right for me?
*Ask 3 Questions is based on Shepherd et al. Three questions that patients can ask to improve the quality of information physicians give about treatment options: A cross-over trial. Patient Education and Counselling, 2011;84:379-85